A summary of some of the pressing public health issues facing Georgia in 2024.
OPIOID CRISIS
Drug overdoses and deaths across the United States have been rising in recent years and media coverage of the opioid crisis is at a high. Deaths began rising in the 90s as physicians began prescribing opioids at a higher rate for medical treatment. While opioids can be a useful tool for pain treatment, they can quickly become addictive and deadly. Through scientific research, we can understand that addiction is not a moral failure, but rather a medical disorder that impacts the functioning of the brain and behavior.
The second wave of overdose deaths came as prescriptions ran out and those who were already addicted began to turn to heroin and the illicit drug market. The third wave of overdose deaths and the current topic of debate on a national stage is concerned with the use of Fentanyl. The drug is 50 times stronger than heroin making it lethal in even small doses. Additionally, Fentanyl is cheap to produce, leading illicit drug manufacturers to lace a multitude of other drugs with it. The only way to determine if a drug is laced with Fentanyl is with test strips which are cheap and give fast results.
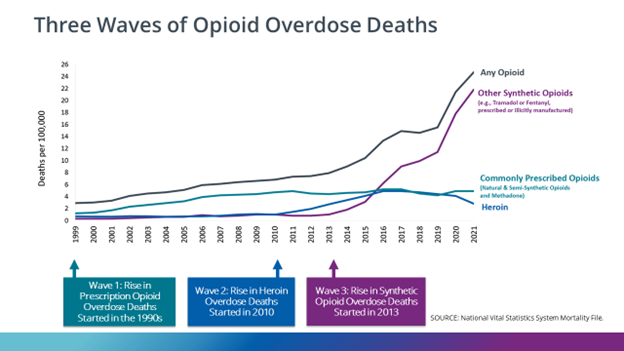
Since 2019, the drug overdose rate in Georgia has increased by 61.9% from 2019 to 2021 and emergency department visits for overdoses have surpassed 27,000 annually in 2021. Opioid use disorder and fatal overdoses cost the state an estimated annual $21 million. In response to the increase in overdoses, Naloxone has been approved for over-the-counter purchase. The drug is sold in a variety of forms and can be used to temporarily stop the effects of an opioid overdose and allow the patient to resume breathing.
The state is set to receive $636 million in pharmaceutical lawsuit settlement funding. According to the Memorandum of Understanding from the agreement, 25% will be distributed to local governments. While funds have already started to be allocated to Medicated Assisted Treatment, detox bed space, stigma reduction, and naloxone access, leaders have yet to divulge long-term plans for the funding distributed over 18 years. Transparency and data tracking of funding must be set up to ensure that the funding received goes back to the most impacted communities.
Learn More ABOUT the Opioid Crisis
GDPH naloxone- https://dph.georgia.gov/stopopioidaddiction/opioid-basics/naloxone
GDPH settlements- https://opb.georgia.gov/ohsc/opioid-settlement-agreements
GBPI Settlement funding- https://gbpi.org/opioid-settlement-funding-presents-opportunity-to-address-georgias-drug-overdose-epidemic/
RURAL HEALTHCARE
The rural-urban health divide is widening, putting more than 46 million Americans at risk of severe health complications. Rural areas face many healthcare access problems such as hospital closures, provider reduction, specialty care, and minority healthcare resources. Additionally, rural populations face other public health challenges such as access to transportation or healthy food options. Solutions for these challenges include ensuring telemedicine is covered, specialized mobile clinics, loan repayment programs for rural healthcare workers, expansion of practice for certain professionals, and malpractice requirement reforms.
Rural Georgians face higher death rates due to strokes, cancer, heart disease, and motor vehicle accidents; higher rates of smoking; increased rates of chronic disease; and an epidemic of poor maternal health outcomes. Additionally, hospitals in rural Georgia have continued to close in the past decade, the third highest level in the country. To bridge his healthcare gap and increase access to capable providers across the state, the General Assembly should allow physician assistants and advanced practice registered nurses to practice to the full extent of their training and expand broadband access.
Learn More about Rural Healthcare
GBPI safety net- https://gbpi.org/new-legislation-and-continued-failure-to-expand-medicaid-put-georgias-health-care-safety-net-on-uncertain-path/
RHI stats- https://www.ruralhealthinfo.org/states/georgia
GAO problems- https://www.gao.gov/blog/why-health-care-harder-access-rural-america
MEDICAID EXPANSION
Medical insurance is essential to ensuring people can access the preventative care, screenings, and medical treatments that they need to live a happy and healthy life.
Georgia is one of ten states that have not approved the expansion of Medicaid. Right now, pandemic Medicaid access is being slowly unwound, the state is launching the new Pathways coverage program, and is establishing a state-based insurance marketplace. A major component of the Pathways program is placing work requirements as a condition for coverage. This is touted as a viable way to increase employment rates and help people to be more self-sufficient without government assistance. However, all the evidence surrounding work requirements points to the contrary. Work requirements utilize reporting systems that can be confusing and difficult to access if there is no broadband internet access, leaving already vulnerable populations in a precarious situation. Most Medicaid enrollees are already working, and work requirements lead to coverage loss without increasing employment rates. Completing all these goals at once creates unnecessary risk to the coverage of low-income individuals, and costs Georgia money. Prioritizing expanding Medicaid and eliminating work requirements would allow the state to utilize federal funding and prevent unnecessary gaps in coverage.
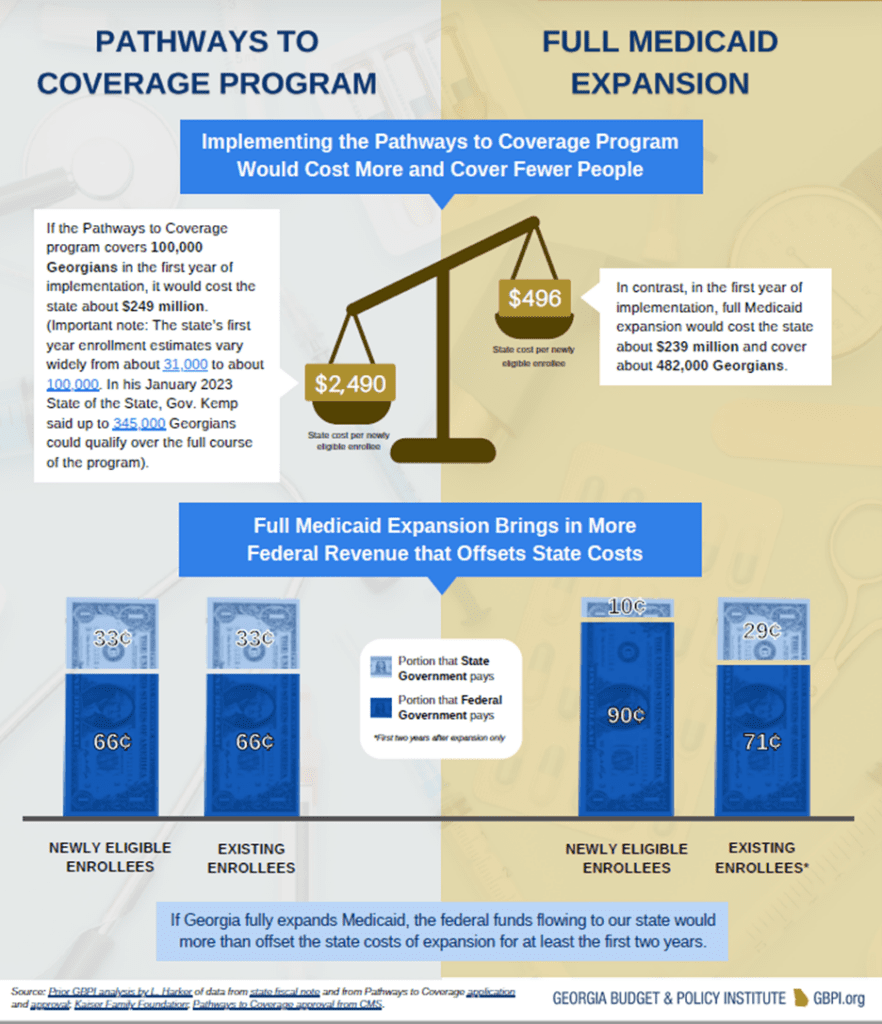
Learn moRE ABOUT Medicaid Expansion
KFF expansion map- https://www.kff.org/medicaid/issue-brief/status-of-state-medicaid-expansion-decisions-interactive-map/
KFF work requirements- https://www.kff.org/medicaid/issue-brief/an-overview-of-medicaid-work-requirements-what-happened-under-the-trump-and-biden-administrations/
